Operations, Practice Management
4 Ways to Increase Practice Revenue—When Vision Plans Won’t
“I want to increase revenue coming into the practice, but I can’t raise my fees because the insurance company only pays what is contracted in their plan.” That was some of the feedback I received after writing an article a couple months ago about increasing net without cutting costs – in particular staff costs.
What can we do as practice owners to increase revenue in a system where the entity paying for our services has set our reimbursement?
There are other ways to increase revenue without approaching the insurance question that was mentioned in the previous article. Those are listed here:
- Improve patient flow. Can you work your schedule to add one more patient slot in your morning schedule and your afternoon schedule? The revenue from those patients will improve your net.
- Make sure your appointment book stays full. Encourage patients to refer friends and family. Make sure the staff knows the importance of patient recall.
- Hold off on new equipment purchases until the net improves, especially equipment that does not immediately generate revenue.
- Reduce the number of frames in inventory.
- Reduce or eliminate contact lenses in inventory. Consider not stocking contact lenses and ordering when needed.
- Study all categories of cost and cut in other areas, if possible.
For purposes of this article, let’s tackle the insurance question head-on. What can we do when our reimbursement is fixed, and no matter how high we raise fees, we still get paid the same? Let’s explore a few alternatives.
Differentiate
One alternative is to provide services and products that are not covered by most insurance plans. Things like specialty contact lenses, sports vision and vision therapy are generally not covered by most insurance plans, and you will be able to generate more revenue in these areas. Making your practice a leader in a specialty can generate increased income.
Highlight Your Best Patients
Review your schedule daily and highlight those patients who in the past have used your products and services and have paid for the better frame or the larger quantity of contact lens supplies. Make sure their experience with you is great at every visit
Have your opticians review what they have purchased in the past and lead with that. For example, if the patient is a big fan of Prada frames, and has bought several in the past, make sure the optician shows them the latest Prada offerings. Your “good” patients are more likely to purchase more than “what the plan pays for.” They will upgrade to better materials and are more than likely to buy second pairs that are not covered by their plan.
Review Insurance Plan Yearly & Negotiate
Once a year, review all the insurance plans you accept and what they reimburse. Take the lowest-paying plans and contact them with a request for better reimbursement, if you can. What I mean by “if you can,” is that if your schedule is consistently booked then you have leverage to renegotiate with an insurance company. You have to be able to walk away from the plan at contract’s end to make this strategy effective. Inform the plan that if fees aren’t raised by the next plan cycle, then you will not stay with the plan.
If you are booked out, and your schedule is consistently full, this strategy should not hurt you as you can fill the slots lost to that plan by the patients you have from your other plans. On the other hand, if you consistently have openings in your schedule, then you need to be wary of reducing your revenue even more. After all, some revenue is better than none. Also, a busy office sends a message to patients that they have come to a good place. How do you feel walking into a restaurant for dinner and seeing you are the only ones there versus seeing a full house?
Drop Your Lowest-Reimbursing Plan at the End of the Year
One variation of the strategy above is to drop your lowest reimbursing plan at the end of the year. Another is to drop the least-utilized plan. If negotiating is uncomfortable for you, then just make the decision yourself and drop a plan. If you choose the lowest-paying plan, least utilized or most difficult to work with, it generally will make you and your staff happier, and if researched correctly, may actually be more beneficial to the practice bottom line in the long run.
Let’s look at some estimates of what would happen in the scenario listed above. The numbers listed in the table are random and do not reflect true reimbursements. You can plug in your own information on this Excel page to guide you in making a decision.
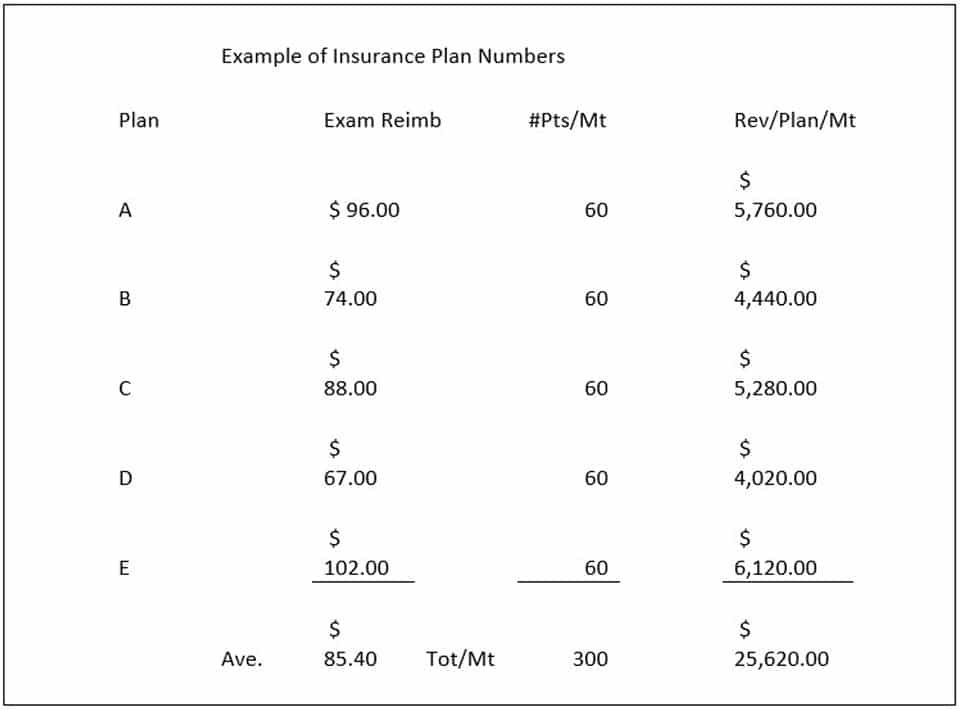
In the example above we are going to drop the lowestreimbursing plan, so we will drop plan D. What happens? You lose all those patients for the next month and their $4,020 in exam revenue, so your practice suffers a reduction in revenue of 15.7 percent. This is not good if those patients are not replaced with patients from your remaining plans.
What does it take to replace the patients you lost and still have the same revenue? You need to replace the $4,020 that the lowest-paying plan was paying you. The remaining four plans now average $90 per exam. You need to replace 45 of the 60 patients you lost to break even. Of course, breaking even is not the goal, but more than likely over time you will go back to filling up your appointment schedule but with better-paying patients, or rather, betterpaying insurance plans.
The example above is overly simple since it is only five plans and reimbursement for exam fees only. Your practice and your insurance plans are much more complicated since they involve multiple plans and reimbursement for multiple fees and services. It requires some study and faith that you will replace those patients that you lose when you drop a plan.
Finally, your practice does not have to take every insurance plan available to patients. It can be beneficial to pare back on plans that are not as beneficial to your revenue as others, just make sure your practice is in a position to do so before making changes.

